Sex has many different meanings for different people, but communication is always key to making it a pleasurable experience. Having type 1 diabetes (T1D) can make that communication more awkward for some, but it certainly doesn’t have to ruin your moment! If you’re looking for a breakdown of how to get diabetes out of the way so that the fun can begin, you’ve come to the right page.
First and foremost, know that you’re likely to experience changes in your blood sugar. You could experience a spike in your blood sugars from hormones, so keep your insulin handy if you don’t think it will level off. Conversely, you could see a drop in your blood sugars from the activity, so have some low snacks at the ready. In fact, your low snacks could be a part of your sexy time (chocolate-covered strawberries, anyone)? Let your partner know that you have T1D, how it works, and that the candy undergarments in the nightstand are for low blood sugars only (or have another snack ready).
If you know ahead of time that sex is in your very-near future, you may want to decrease your basal insulin, especially if you use a pump and can take advantage of a temp basal. If your device has tubing you might even disconnect from your pump entirely. How much you reduce your insulin is dependent on your body and your endocrinologist may be able to make a suggestion based on your correction factor and patterns. Don’t be afraid to ask for input when you’re getting your next insulin refill: that’s what they’re there for!
Before you get down to business, you ought to test or check your continuous glucose monitor CGM data so that you know where you’re starting. If you need to get some glucose in your system, better to do it before you’re already low. If you haven’t mentioned that you have diabetes by this point when the heat is rising, now is a good time. You can even turn it into a silly line such as, “I hope you have a sweet tooth.” Laughter banishes awkwardness and facilitates bonding—and if you’re really smooth it will be just plain sexy.
Just remember, diabetes is a complex condition and you get to decide how much you want to disclose. You can keep it as simple as, “I have type 1 diabetes, which is an autoimmune condition that makes me have to monitor and regulate my own blood sugar levels. If they go high, I need to inject insulin. If I go low, I need to ingest sugar.” Alternately, you can take a few minutes to explain in more detail. It’s up to you.
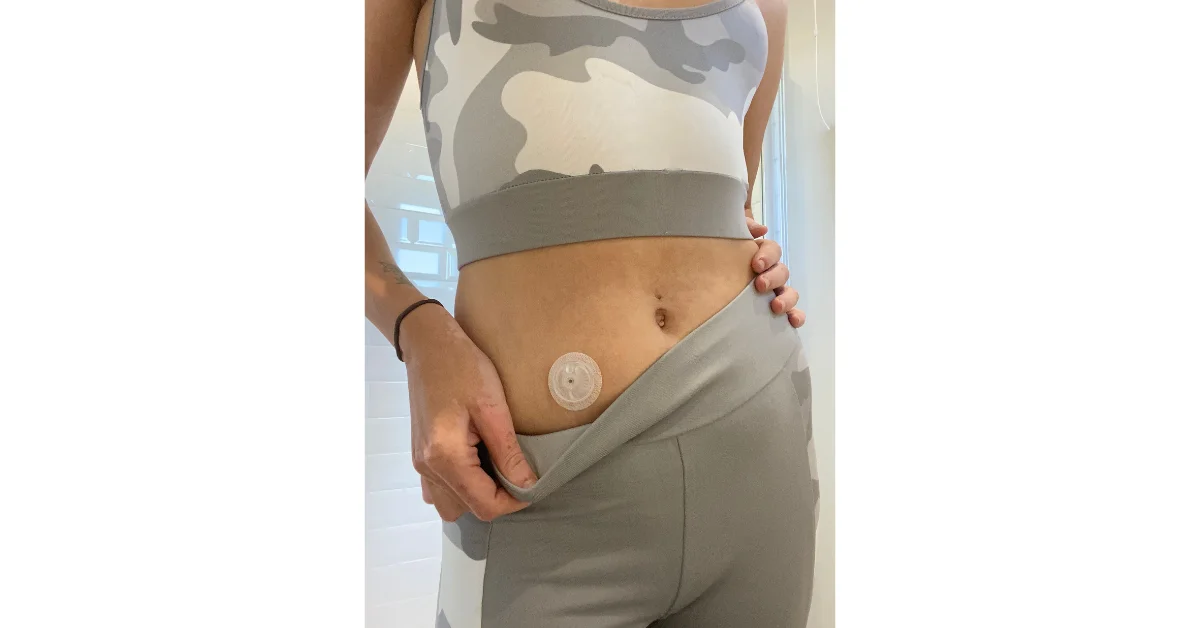
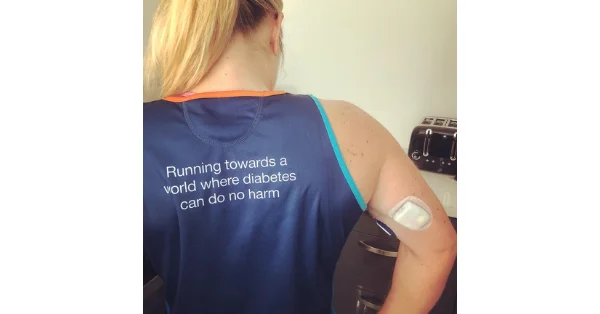
Now, a word on getting your clothes off and sexy on: if you wear any devices, whether a (CGM), a pump, or both, you may want to bring them to your partner’s attention for a purely logistical reason. It’s a pain and a hassle when medical devices get ripped off and out. If your partner is aware of the CGM on your arm or the pump on your abdomen, then they can be more cautious, whether you’re getting undressed or you’re in the act.
If you’ve done all of the above and you end up with a low anyway, be sure to address it immediately. Getting a low blood sugar while in the throes of passion is inconvenient and can be frustrating, but it gets worse if you try to ignore it. Maybe consider it extended foreplay. Did you bring enough candy to share?
Finally, know that if your blood sugars have been running low or high, it may affect your desire to have sex. It could even affect your performance. For instance, some people with T1D may find it more difficult to get aroused or maintain arousal. It’s okay to take a break and try again later or do different sexual acts which accommodate any given difficulties.
I know I mentioned this earlier, but I want to emphasize that this is your body, your diabetes, and your sexual pleasure that we’re discussing. You and your partner both should feel respected throughout this process. Your partner should be supportive of whatever you need to do for your health. If they are not, then they’re not a good sexual partner and they belong in your rearview. On that note, if any suggestions above don’t work for you, by all means, don’t feel pressured to employ them. Conversely, if you did find these tips helpful, I’m overjoyed! Do what keeps you and your partner safe, and go get yourself some sugar.

Danielle Martin-Jensen
Danielle was diagnosed with type 1 diabetes in August 2016. Since then she has written guest articles for College Diabetes Network (CDN) on body positivity and study abroad, participated in a livestream panel discussion on study abroad for a CDN-Mobility International collaboration, and written an article for DMP on how to manage diabetes during intimacy. She manages her diabetes with the Dexcom G5 and Omnipod. Her interests include travel, science, and podcasts.